Personalized Care
View GalleryWho will be treating me?
YOUR CARE TEAM
A team of highly trained medical professionals will be involved in your care during radiation therapy. This team is led by a radiation oncologist, a doctor who specializes in using radiation to treat cancer.
Radiation Oncologists
Radiation oncologists are the doctors who will oversee your radiation therapy treatments. These physicians work with the other members of the radiation therapy team to develop and prescribe your treatment plan and make sure that each treatment is given accurately. Your radiation oncologist will also track your progress and adjust the treatment as necessary to make sure you receive the best care. Radiation oncologists help identify and treat any side effects that may occur due to radiation therapy. They work closely with other cancer doctors, including medical oncologists and surgeons, and all members of the radiation oncology team.
Radiation oncologists are the only physicians with the expertise and training to deliver radiation therapy treatments. In addition to college and medical school, five years of additional training are required for radiation oncologists. They receive extensive training in cancer medicine, in the use of radiation to treat disease and in managing any side effects caused by radiation. Once they pass an examination by the American Board of Radiology, radiation oncologists are board certified.
Radiation Therapists
Radiation therapists work with radiation oncologists to give the daily radiation treatment under the doctor’s prescription and supervision. They maintain daily records and regularly check the treatment machines to make sure they are working properly.
Radiation Oncology Nurses
Radiation oncology nurses work with every member of the treatment team to care for you and your family before, during and after treatment. They will explain the possible side effects you may experience and will describe how you can manage them. They will assess how you are doing throughout treatment and will help you cope with the changes you are experiencing.
Medical Physicists
Medical physicists work directly with the radiation oncologist during treatment planning and delivery. They oversee the work of the dosimetrist and help ensure that complex treatments are properly tailored for each patient.
Medical physicists develop and direct quality control programs for equipment and procedures. They are trained with advanced degrees and appropriately credentialed to provide this important service. These professionals make sure the equipment works properly by taking precise measurements of the radiation beam and performing other safety tests on a regular basis.
Dosimetrists
Dosimetrists work with the radiation oncologist and medical physicist to carefully calculate the dose of radiation to make sure the tumor gets the prescribed amount. Using computers, they develop an optimized treatment plan that can best destroy the tumor while sparing the healthy tissue.
Other members of the treatment team may include social workers, nutritionists, patient navigators, radiation engineers, physical therapists, radiation data managers, dentists and clerical staff . In cases where radiation is used in combination with chemotherapy or surgery, a coordinated multidisciplinary team often extends beyond the radiation treatment team to include health care professionals from medical oncology and surgery.
What happens before, during and after treatment?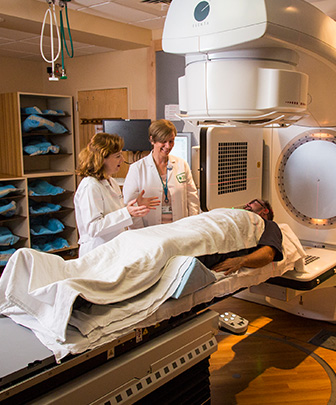
Once a diagnosis has been made, you will probably talk with your primary care physician along with several cancer specialists, such as a surgeon, a medical oncologist and a radiation oncologist. You will want to ask these doctors about all your treatment options. In many cases, but not all cases, your cancer will need to be treated by using more than one type of treatment.
If it is determined that you would benefit from radiation oncology, your radiation oncologist will review any scans that have been ordered, including CT scans, MRI scans and PET scans, and complete a thorough examination. He or she will then discuss with you the potential benefits and risks of radiation therapy and answer your questions.
BEFORE RADIATION TREATMENT
During your first visit, your radiation oncologist will evaluate your need for radiation therapy and its likely results. This includes reviewing your current medical problems, past medical history, past surgical history, family history,medications, allergies and lifestyle. The doctor will also perform a physical exam to assess the extent of your disease and judge your general physical condition. You may also be seen by a medical student, a resident (radiation oncologist in training), a nurse practitioner, a physician’s assistant or a nurse.
Simulation
To be most effective, radiation therapy must be aimed precisely at the same target or targets each and every time treatment is given. The process of measuring your body and marking your skin to help your team direct the beams of radiation safely and exactly to their intended locations is called simulation. During simulation, your radiation oncologist and radiation therapist place you on the simulation machine in the exact position you will be in during the actual treatment. Your radiation therapist, under your doctor’s supervision, then marks the area to be treated directly on your skin or on immobilization devices. Immobilization devices are molds, casts, headrests or other devices that help you remain in the same position during the entire treatment. The radiation therapist marks the immobilization devices and/or your skin with either a bright, temporary paint or a set of small, permanent tattoos. Often, a special treatment planning CT scan is done to help with the simulation and treatment planning. This CT scan is in addition to your diagnostic CT scan. Your radiation oncologist may request that special blocks or shields be made for you. These blocks or shields are put in the external beam therapy machine before each of your treatments and are used to shape the radiation to your tumor and keep the rays from normal tissue. Multi-leaf collimators, shaping devices located in the head of the linear accelerator itself, may also be used to shape the beam and achieve safe delivery of your radiation treatment.
Treatment Planning
Once you have finished simulation, your radiation oncologist and other members of the treatment team review information obtained during simulation along with your previous medical tests to develop a treatment plan. A sophisticated treatment-planning computer and associated software may be used to help design the best possible treatment plan. After reviewing all of this information, your doctor will write a prescription that outlines exactly how much radiation you will receive and to what parts of your body.
Quality Assurance Before Treatment
Once your doctor approves the radiation therapy plan in treatment planning the members of the radiation treatment team work together to ensure that your specific treatment plan works correctly on the linear accelerator before treatment begins. A ‘dry run’ is often completed for more complex treatments by a medical physicist to ensure that the radiation treatment designed for you is as accurate and as safe as possible.
DURING EXTERNAL BEAM RADIATION THERAPY TREATMENTS
When you undergo external beam radiation therapy treatment, each session is painless, just like getting an X-ray. The radiation is directed at your tumor from a machine located away from your body, usually a linear accelerator. External beam radiation is noninvasive, unlike surgery, which is an invasive process. One of the benefits of radiation therapy is that it is usually given as a series of outpatient treatments (meaning you don’t have to stay in the hospital). You may not need to miss work or experience the type of recuperation period that may follow other treatments. The radiation therapist will give you your external beam treatment following your radiation oncologist’s instructions.
It will take five to 15 minutes for you to be positioned for treatment and for the equipment to be set up. If an immobilization device was made during simulation, it will be used during every treatment to make sure that you are in the exact same position every day. Time spent in the treatment room may vary depending on the type of radiation, but it generally ranges from 10 to 40 minutes. Once you are positioned correctly, the therapist will leave the room and go into the control room next door to closely monitor you on a television screen while giving the radiation. There is a microphone in the treatment room so you can always talk with the therapist if you have any concerns. The machine can be stopped at any time if you are feeling sick or uncomfortable.
The radiation therapist may move the treatment machine and treatment table to target the radiation beam to the exact area of the tumor. The machine might make noises during treatment that sound like clicking, knocking or whirring, but the radiation therapist is in complete control of the machine at all times. Your radiation oncologist monitors your daily treatment and may alter your radiation dose based on these observations. Also, your doctor may order blood tests, X-rays and other tests to see how your body is responding to treatment. If the tumor shrinks significantly, another simulation may be required. This allows your radiation oncologist to change the treatment to destroy the rest of the tumor and spare even more normal tissue.
Sometimes a course of treatment may need to be interrupted for a day or more. This may happen if you develop side effects that require a break in treatment. These missed treatments may be made up by adding treatments at the end. However, it is best to try to arrive on time and not miss any of your appointments. Treatments are usually scheduled five days a week, Monday through Friday, and continue for one to 10 weeks. The number of radiation treatments you will need depends on the size, location and type of cancer you have, the intent of the treatment, your general health, and other medical treatments you may be receiving.
A portion of your external radiation therapy may be directed at the tumor and surrounding tissues at risk for harboring microscopic cancer cells. This might be followed by shrinkage of the volume of tissue treated to the tumor area itself, since this area may require a higher dose to eliminate the cancer cells. This is called a boost.
In some cases, a patient may receive chemotherapy and radiation therapy at the same time. The chemotherapy may be delivered weekly, every three weeks or at some schedule determined by the medical oncologist together with the radiation oncologist. The chemotherapy may work to help sensitize the cancer cells in the target area to the radiation therapy and may also travel elsewhere in the body to help destroy or reduce microscopic cancer cells. Your treatment team will help coordinate these therapies and care for potential side effects.
Weekly Checkups
During radiation therapy, your radiation oncologist and nurse will see you regularly to follow your progress, evaluate whether you are having any side effects, recommend treatments for those side effects (such as medication) and address any concerns you may have. Your doctor may also make changes in the schedule or treatment plan depending on your response or reaction to the therapy. Your radiation oncology team may gather on a regular basis with other health care professionals to review your case to ensure your treatment is proceeding as planned. During these sessions, all the members of the team discuss your progress and any concerns.
Quality Assurance During Treatment
During your course of treatment, correct positions of the treatment beams will be regularly verified with images made using the treatment beam itself. These images (called port films, beam films or portal verification) represent an important quality assurance check but do not evaluate the tumor itself. Depending upon what kind of treatment you receive and what your doctor thinks will work best, the type of images used (e.g., X-ray, CT scan, ultrasound, etc.) may vary. These images assure your radiation oncologist that the treatment setup accurately matches the intended target.
AFTER TREATMENT FOLLOW-UP
After treatment is completed, follow-up appointments will be scheduled so that your radiation oncologist can make sure your recovery is proceeding normally. Your radiation oncologist, in concert with other members of your team, may also order additional diagnostic tests. Reports on your treatment may also be sent to the other doctors helping treat your cancer. As time goes by, the number of times you need to visit your radiation oncologist will decrease. However, you should know that your radiation oncology team will always be available should you need to speak to someone about your treatment.
How should I care for myself during radiation therapy?
Get plenty of rest. Many patients experience fatigue during radiation therapy, so it is important to make sure you are well rested. If possible, ask friends and family to help out during treatment by running errands and preparing meals.
This will help you get the rest you need to focus on fighting your cancer. If you need more help, ask your social worker or nurse to give you information on a local cancer support group or other resources. Volunteers may be able to help.
Even though it is important to recognize when you might need some rest, there is good evidence to suggest that some physical activity during treatment can help decrease the fatigue. For example, many patients feel a daily walk helps decrease some of their treatment-related fatigue. Ask your radiation oncologist what the best form of daily exercise might be for you.
Follow your doctor’s orders. In many cases, your doctor will ask you to call if you develop a fever of 101.0 F or higher. Be sure to read your instructions as far as caring for yourself during treatment.
Eat a balanced, nutritious diet. A nutritionist, nurse or doctor may work with you to make sure you are eating the right foods to get the vitamins and minerals you need. With certain types of radiation, you may need to change your diet to minimize side effects. You should not attempt to lose weight during radiation therapy since you need more calories due to your cancer and treatment.
Stay hydrated. In some cases, you may be at risk of becoming dehydrated during treatment. Helpful fluids may include flat soda, JELL-O, juice, sorbet, broth and water. Discuss with your doctor what strategies will work best.
Treat skin exposed to radiation with extra care. The skin in the area receiving treatment may become red and sensitive, similar to a sunburn. Your radiation oncology nurse will review specific instructions for caring for your skin with you. Some guidelines include:
- Clean the skin daily with warm water and a mild soap recommended by your nurse.
- Avoid using any lotions, perfumes, deodorants or powders in the treatment area unless approved by your doctor or nurse. Avoid products containing alcohol, which may dry your skin.
- Avoid putting anything hot or cold on the treated skin. This includes heating pads and ice packs.
- Stay out of the sun. If you must be outdoors, wear a hat or clothing to protect your skin. After treatment, use sunscreen with an SPF of at least 30 or higher.
Seek out support. There are many emotional demands on you during your cancer diagnosis and treatment. It is common to feel anxious, depressed, afraid or hopeless. It may help to talk about your feelings. To find a support group in your area, ask your radiation oncology nurse. There are many groups that meet in person, over the phone or on the Internet.
Some support organizations can even help you manage financial issues, such as insurance and co-pays.