UW faculty receive NIH award to expand access to radiation treatment in low- and middle income countries
We are pleased to announce the award of a major research grant from the National Cancer Institute. This award of $2.9 M will support the development of a cost-effective technology for radiation therapy that is specifically designed for low- and middle-income countries (LMICs). The investigators, under the leadership of UW professor Dr. Eric Ford, will address the urgent need of more targeted radiation therapy by developing a simple and cost-effective technology to deliver high-quality radiotherapy in the frequently resource-limited facilities of LMICs.
As many gains have been made in LMICs against infectious diseases and other health challenges, cancer has emerged as a major public health threat in these countries. More than half of all cancer patients world-wide live in LMICs, and at least half of these patients are expected to need radiation therapy to treat their disease. However, there is a profound lack of access to advanced radiation therapy technologies that allow normal tissues to be effectively protected from radiation, because in many LMICs only simple radiation machines are available, such as Cobalt 60 units. These treatment machines cannot provide precision radiation therapy techniques, such as intensity-modulated radiation therapy (IMRT), to target the tumor precisely and steer the beam away from nearby normal tissues. This increases the risk of life-long normal tissue complications for patients in LMICs. In addition, because of the difficulty in protecting normal tissues, the treatment dose to the tumor frequently has to be limited. This reduces the chance of treatment success.
With this NIH award, and together with clinical and industry partners in India, the team will develop a prototype system as an external attachment (Compensator System) to simple radiation treatment units. The prototype is expected to be ready for clinical testing in two years. The team has simulated the Compensator System’s radiation dose maps and compared them with dose maps of the more advanced targeted treatments used in U.S. facilities. One of these is shown below:
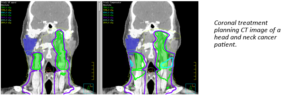 The dose maps are very similar between the left image (IMRT with 6 MV x-rays from a U.S. linear accelerator) and the right image (simple Cobalt 60 beam with the Compensator). Both show high dose to the target areas (green areas surrounded by the green treatment dose line) and very low dose to the right parotid gland tissue (blue with the yellow the low dose line of 26 Gy touching only a small part of the bottom of the parotid gland). This will protect the patient’s saliva and, at the same time, treat the tumor region to an adequate treatment dose.
The dose maps are very similar between the left image (IMRT with 6 MV x-rays from a U.S. linear accelerator) and the right image (simple Cobalt 60 beam with the Compensator). Both show high dose to the target areas (green areas surrounded by the green treatment dose line) and very low dose to the right parotid gland tissue (blue with the yellow the low dose line of 26 Gy touching only a small part of the bottom of the parotid gland). This will protect the patient’s saliva and, at the same time, treat the tumor region to an adequate treatment dose.
“Reducing the dose to the parotid gland preserves patients’ saliva function, prevents a permanent dry mouth for the rest of their lives, and thereby reduces the chance of tooth decay and poor nutrition after radiation. This improves the lives of head-and-neck-cancer patients. The same principle of dose reduction to normal tissues can be applied to the treatment for many other cancers.” says Mayr.
Dr. Eric Ford is Professor and medical physicist in the University of Washington School of Medicine Department of Radiation Oncology with extensive experience in technology development including 4-dimensional CT and other advanced technologies. The UW team includes radiation oncologist physician faculty Drs. Nina Mayr and Shilpen Patel, certified dosimetrist Patricia Sponseller, and a team of postdoctoral researchers and students. UW partners include Patterson Cancer Center and Panacea Medical Inc. in India and co-investigators Drs. S. Vijayaraghavan, G.V. Subrahmanian and K. Govindarajan, Adam Shulman from Radiating Hope, and Dr. D. Brown from the University of California San Diego.
This research will be another contribution to the University of Washington’s important work in global health in the Department of Global Health and many collaborators and Departments around the UW campus. “The severe limitations in radiation therapy technologies are not easily and quickly resolved in LMICs”, says Dr. Judith N. Wasserheit, Professor and Chair of the UW School of Medicine’s Department of Global Health [https://globalhealth.washington.edu/], “Therefore an innovative technology solution to overcome this profound gap brings hope to improve cancer treatment and save lives among underserved tumor patients around the world.”
“Initial results are very promising,” says Ford. “Imagine a technology that is 10 or even 100 times cheaper than what we have today. Imagine the impact this can have for so many people who really have nothing.”
