
Investigators
Summary
Eligibility: Patients with stage IIB or stage III non-small cell lung cancer getting chemoradiation Learn More
Clinical goal: Decrease lung toxicity from radiation treatment, and improve tumor control
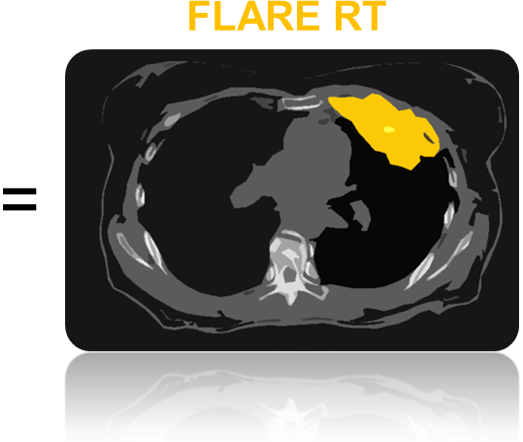
Intervention: Functional Lung Avoidance and Response-adaptive Escalation (FLARE) Radiation Therapy (RT)
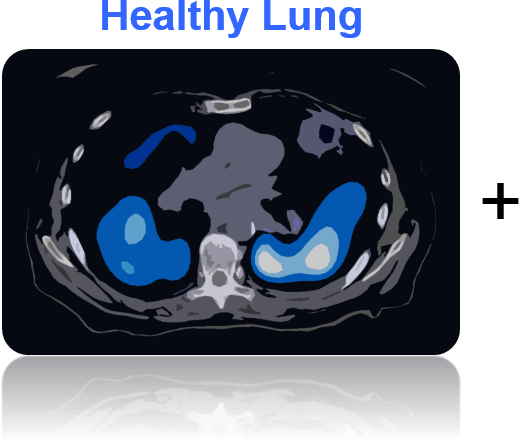
Healthy lung imaging: Pre-radiation treatment scans to analyze perfusion and ventilation in the lung and define radiation avoidance regions
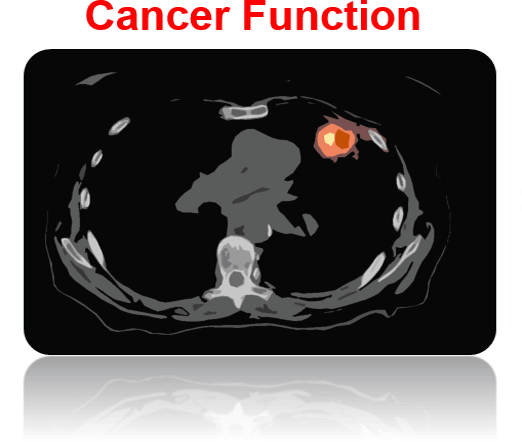
Cancer function imaging: Mid-radiation treatment scan to analyze tumor response to therapy, and intensify dose if tumor does not appear to be responding well
Lung cancer is the leading cause of cancer deaths in the United States. Survival rate for patients with lung cancer is only 17.4% overall.
Radiation therapy is often used to treat lung cancer (either alone or in combination with chemotherapy and surgery). However, lung cancer sometimes comes back after treatment. Using advanced cancer imaging, we are predicting which tumors are more likely to come back, and intensifying treatment to those tumors. This also helps spare excess radiation to patients whose tumors are not likely to come back.
Beyond curing more lung cancers, we are also decreasing side effects from treatment, by using specialized lung imaging to avoid treating healthy parts of the lung with radiation. Healthy lung sparing allows for safer treatment intensification in select patients.
By imaging and mapping out the healthy lung tissue (blue in left figure), and imaging and mapping out lung tumors that are at high risk of coming back after treatment (red in middle figure), we are developing radiation treatments (yellow in right figure) that cure lung cancers without causing excess side effects. Adding imaging of healthy lung and imaging of cancer function together produces a more personalized therapy, known as FLARE RT.
